Atrial flutter vs a fib9/4/2023  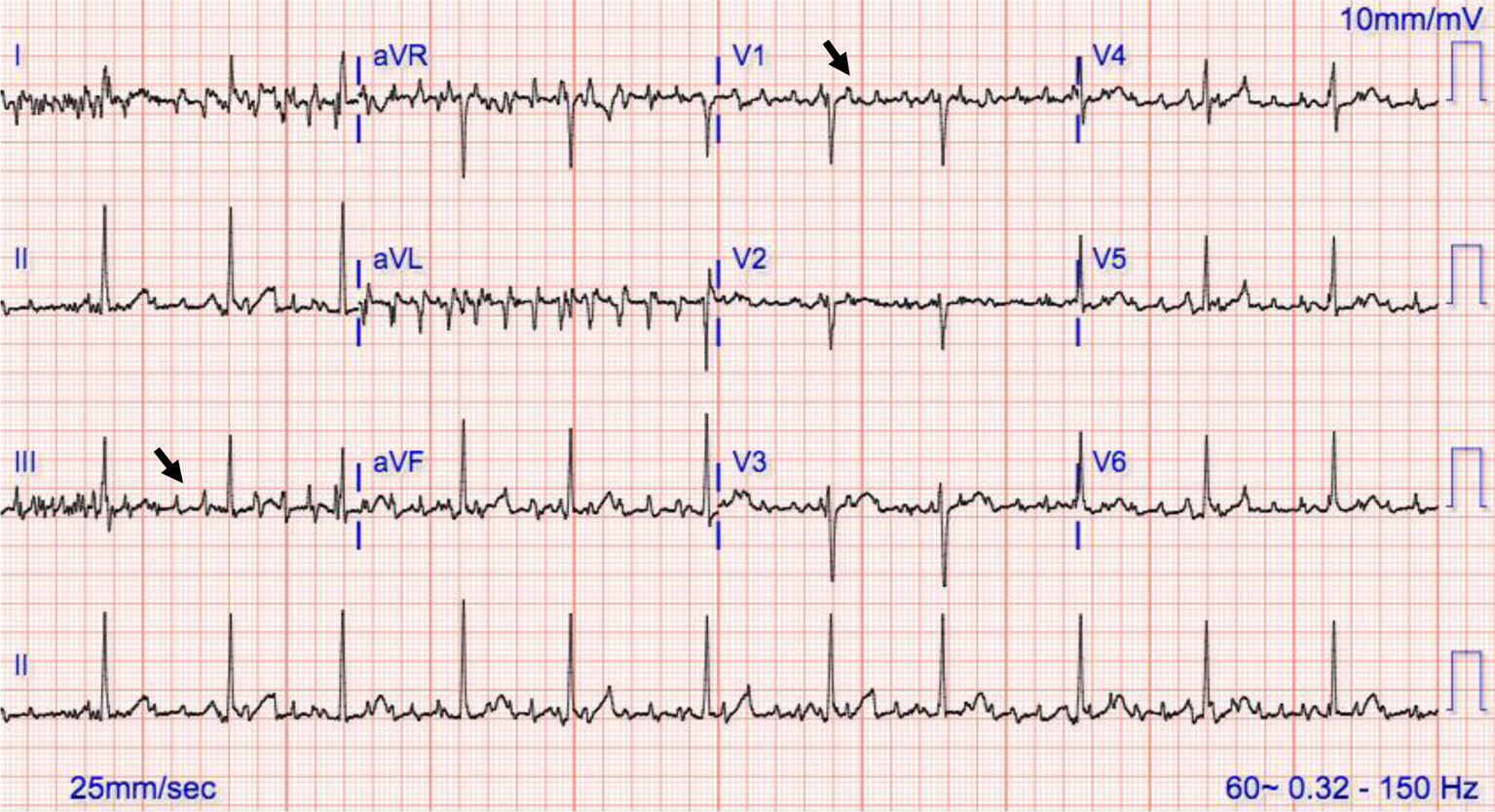
Stroke arrhythmia atrial fibrillation atrial flutter. Patients with atrial flutter faced a lower risk of ischemic stroke than patients with atrial fibrillation. 
Within 1 year, 65.7% (95% CI 64.9%-66.4%) of patients with flutter converted to fibrillation but remained at a lower risk of ischemic stroke (hazard ratio. After adjustment for demographics and stroke risk factors, flutter was associated with a lower risk of stroke compared with fibrillation (hazard ratio. The annual incidence of ischemic stroke in patients with flutter was 1.38% (95% confidence interval 1.22%-1.57%) compared with 2.02% (95% CI 1.99%-2.05%) in patients with fibrillation. During a mean follow-up period of 2.8 (☒.3) years, we identified 18,900 ischemic strokes. We identified 14,953 patients with flutter and 318,138 with fibrillation. Cox proportional hazards analysis was used to compare the associations of flutter and fibrillation with ischemic stroke after adjustment for demographics and risk factors. There are many similarities between atrial fibrillation and atrial flutter, there are also significant differences.Atrial flutter is an abnormality of. Survival statistics were used to compare incidence of stroke in patients with flutter and patients with fibrillation. In the primary analysis, patients with atrial flutter were censored upon converting to fibrillation in a secondary analysis, they were not. Using inpatient and outpatient Medicare claims data from 2008 to 2014 for a 5% sample of all beneficiaries 66 years of age or older, we identified patients diagnosed with atrial fibrillation and those diagnosed with atrial flutter. Atypical atrial flutter originates from the left atrium or areas in the right atrium, such as surgical scars, and has a variable appearance on ECG in regards to the flutter waves.The aim of this study was to compare the risk of ischemic stroke in patients who have atrial fibrillation and patients who have atrial flutter. This appears as positively-directed flutter waves in the inferior leads. 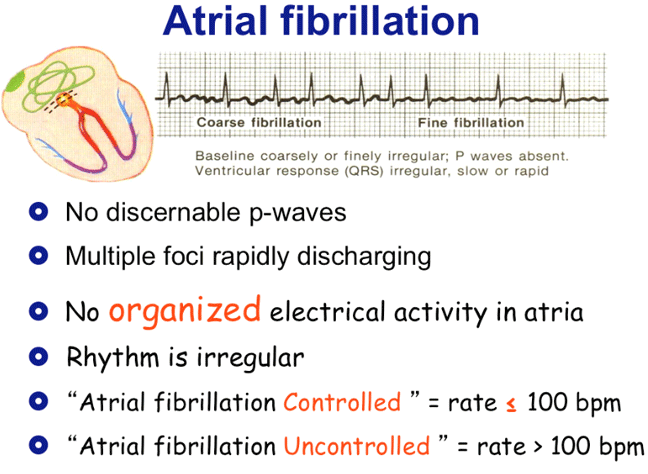
This results in negatively-directed flutter waves in the inferior leads.Īt times, the direction of the circuit can reverse, causing clockwise atrial flutter from the same anatomical location. Typical atrial flutter rotates counterclockwise in direction, from a reentrant circuit around the tricuspid valve annulus and through the cavo-tricuspid isthmus. Also, atrial flutter can be described as “clockwise” or “counterclockwise” depending on the direction of the circuit. In this situation, giving adenosine will transiently slow the ventricular rate, unmasking the atrial flutter waves and allowing a more definitive diagnosis to be made.Ītrial flutter can described as “typical” (type I) or “atypical” (type II) based on the anatomic location from which it originates. When the heart rate is significantly elevated - that is, greater than 150 bpm - it is often difficult to determine atrial flutter from atrial fibrillation, atrial tachycardia or atrioventricular nodal reentrant tachycardia, or AVNRT. Atrial fibrillation (AFib) and atrial flutter (AFL) are the two most frequent types of heart arrhythmias known as atrial tachycardias. This results in the rhythm becoming “irregularly irregular.” There are only two other rhythms that are commonly irregularly irregular, including atrial fibrillation and multifocal atrial tachycardia, or MAT. In this situation, there may be three P waves to one QRS complex, then a quick change to two P waves to one QRS complex, and so on any combination of P waves to QRS complexes can occur. Like AFib, this rapid heartbeat also increases the risk of. As a result, it beats erratically and too fast. The regularity of the QRS complexes frequently present with atrial flutter helps to distinguish it from atrial fibrillation, though atrial flutter with variable conduction of the P waves can also occur. Atrial flutter occurs when certain electrical signals do not reach the ventricles of the heart. AFib or atrial flutter causes the heart to deliver the wrong signals. In this situation, the ventricular (QRS) rate will be exactly 150 bpm and regular.ĬLINICAL PEARL: A narrow complex tachycardia at a ventricular rate of exactly 150 bpm is very commonly atrial flutter. 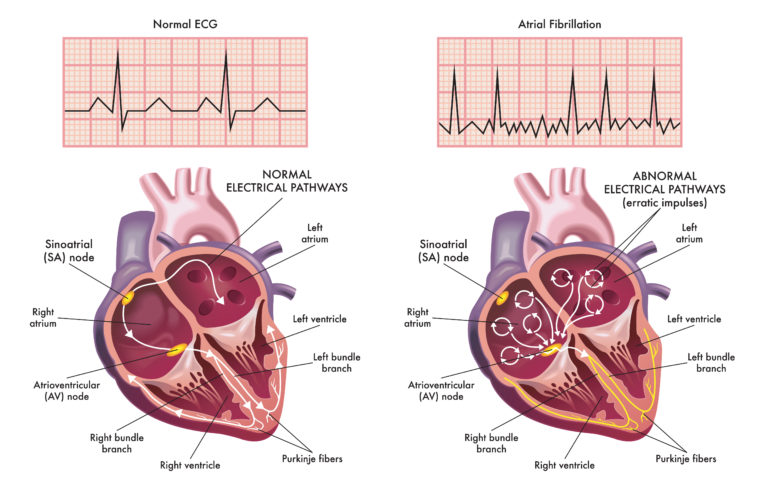
Typically, the atrial rate will be about 300 bpm, and only every other atrial depolarization will be conducted through the AV node. Atrial fibrillation and atrial flutter may come and go or be sustained. Many people with atrial flutter also have episodes of atrial fibrillation. Atrial fibrillation is much more common than atrial flutter. Just as in atrial fibrillation, not all of the P waves are able to conduct through the atrioventricular node, and thus the ventricular rate will not be as fast as the atrial rate. Atrial fibrillation and atrial flutter are more common among older people and people who have a heart disorder. 
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
